Epic workflows move fast. But finding and interpreting payer policies still slows teams down.
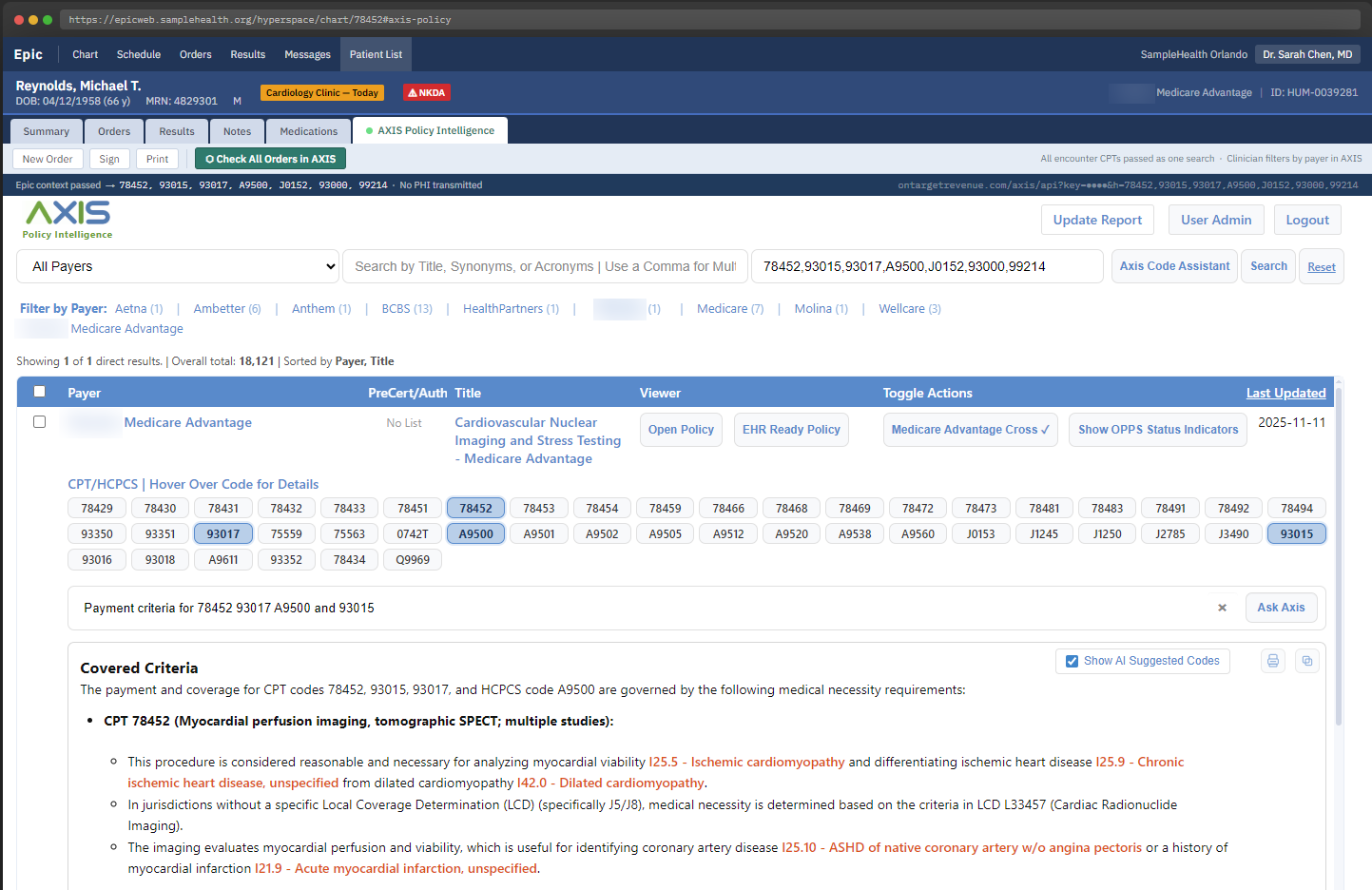
AXIS provides instant access to Medicare and Commercial payer coverage policies, with AI explanations and structured data that can support Epic workflows through APIs and reference links.
Epic is excellent at managing clinical and revenue workflows. But payer policies exist outside the system.
Revenue cycle teams regularly have to:
AXIS aggregates thousands of payer coverage policies nationwide. Instead of navigating dozens of payer websites, teams can:
This makes it faster to determine what the payer actually requires.
Prior authorization requirements are another common policy challenge. Teams often need to confirm whether a CPT requires authorization, what diagnoses qualify, and which payer policy governs the request. Because each payer publishes these requirements differently, staff frequently search multiple websites before they can proceed.
AXIS allows teams to quickly identify the governing policy and review the requirements so authorization decisions can be made with confidence.
Integration options | API Access
Epic workflows can reference AXIS pages that display the governing policy and explanation.
AXIS provides an API that allows external systems to retrieve: